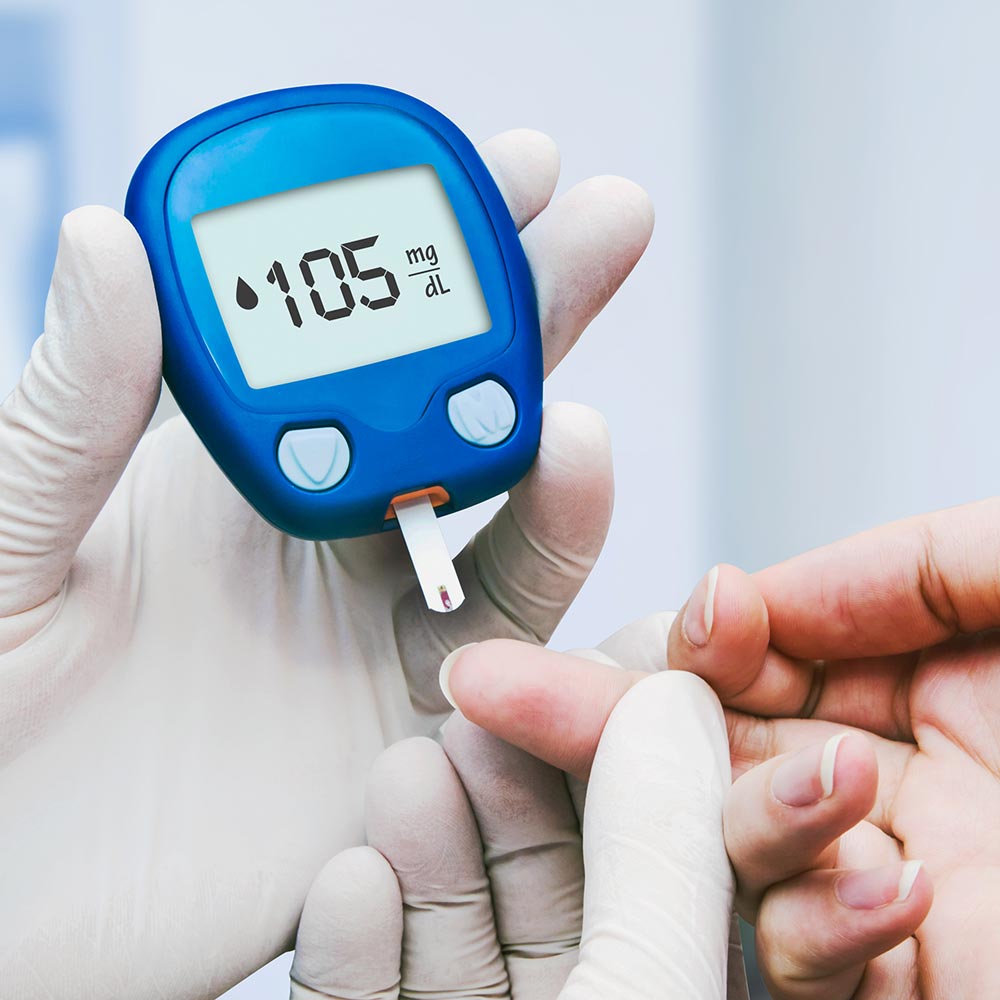
All you need to know about Diabetes in Cameroon;
Prevalence of Diabetes in Cameroon
In Cameroon, the prevalence of diabetes in adults in urban areas is currently estimated at 6 – 8%, with as much as 80% of people living with diabetes who are currently undiagnosed in the population. Further, according to data from Cameroon in 2002, only about a quarter of people with known diabetes actually had adequate control of their blood glucose levels. The burden of diabetes in Cameroon is not only high but is also rising rapidly. Data in Cameroonian adults based on three cross-sectional surveys over a 10-year period (1994–2004) showed an almost 10-fold increase in diabetes prevalence.
Introduction
Diabetes is a chronic (long-lasting) health condition that affects how your body turns food into energy. Most of the food you eat is broken down into sugar (also called glucose) and released into your bloodstream. When your blood sugar goes up, it signals your pancreas to release insulin. Insulin acts like a key to let the blood sugar into your body’s cells for use as energy. If you have diabetes, your body either doesn’t make enough insulin or can’t use the insulin it makes as well as it should. When there isn’t enough insulin or cells stop responding to insulin, too much blood sugar stays in your bloodstream. Over time, that can cause serious health problems, such as heart disease, vision loss, and kidney disease.

Types of Diabetes:
Prediabetes:
Prediabetes is when your blood sugar is higher than it should be but not high enough for your doctor to diagnose diabetes.
Prediabetes can make you more likely to get type 2 diabetes and heart disease.
Type 1 Diabetes
Type 1 diabetes is also called insulin-dependent diabetes. It used to be called juvenile-onset diabetes, because it often begins in childhood.
This type is from auto-immune origin. It happens when your body attacks your pancreas with antibodies. The organ is damaged and doesn’t make insulin.
Your genes might cause this type of diabetes. It could also happen because of problems with cells in your pancreas that make insulin.
Many of the health problems that can come with type 1 happen because of damage to tiny blood vessels in your eyes (called diabetic retinopathy), nerves (diabetic neuropathy), and kidneys (diabetic nephropathy). People with type 1 also have a higher risk of heart disease and stroke.
Treatment for type 1 diabetes involves injecting insulin into the fatty tissue just under your skin.
If you have type 1 diabetes, you’ll need to make changes including:
- Frequent testing of your blood sugar levels
- Careful meal planning
- Daily exercise
- Taking insulin and other medications as needed
Type 2 Diabetes
Type 2 diabetes used to be called non-insulin-dependent or adult-onset diabetes. But it’s become more common in children and teens over the past 20 years, largely because more young people are overweight or obese. About 90% of people with diabetes have type 2.
When you have type 2 diabetes, your pancreas usually creates some insulin. But either it’s not enough or your body doesn’t use it like it should. Insulin resistance, when your cells don’t respond to insulin, usually happens in fat, liver, and muscle cells.
Type 2 diabetes is often milder than type 1. But it can still cause major health complications, especially in the tiny blood vessels in your kidneys, nerves, and eyes. Type 2 also raises your risk of heart disease and stroke.
Type 2 diabetes is often milder than type 1. But it can still cause major health complications, especially in the tiny blood vessels in your kidneys, nerves, and eyes. Type 2 also raises your risk of heart disease and stroke.
People who are obese — more than 20% over their target body weight for their height — have an especially high risk of type 2 diabetes and the health problems that can follow. Obesity often causes insulin resistance, so your pancreas has to work harder to make more insulin. But it’s still not enough to keep your blood sugar levels where they should be.
Gestational Diabetes
Pregnancy usually causes some form of insulin resistance. If this becomes diabetes, it’s called gestational. Doctors often spot it in middle or late pregnancy. Because a woman’s blood sugars travel through their placenta to the baby, it’s important to control gestational diabetes to protect the baby’s growth and development.
Doctors report gestational diabetes in 2% to 10% of pregnancies. It usually goes away after birth. But up to 10% of women who have gestational diabetes get type 2, weeks or even years later.
Gestational diabetes is more of a risk for the baby than the mother. A baby might have unusual weight gain before birth, trouble breathing at birth, or a higher risk of obesity and diabetes later in life. The mother might need a cesarean section because of an overly large baby, or they might have damage to their heart, kidney, nerves, and eyes.
SIGNS AND SYMPTOMS / MANIFESTATION:
Common Symptoms of diabetes include:
- Increased thirst
- Increased hunger
- Frequent urination
- Fatigue
- Blurry Vision
- Cuts or sores that are slow to heal
- Mood changes or irritability
If you do not manage your diabetes and keep your blood sugar levels under control, it can lead to serious or even life-threatening complications over time.
The American Diabetes Association Standards of Care outline the diagnostic criteria for diabetes.
The American Diabetes Standards of Care Diagnostic Criteria for Diabetes |
| Fasting plasma glucose (FPG) ≥126 mg/dL (7.0 mmol/L). Fasting is defined as no caloric intake for at least eight hours. |
| OR |
| 2-hour post prandial (PG) ≥200 mg/dL (11.1 mmol/L) during an oral glucose tolerance test (OGTT). The test should be performed as described by the World Health Organization, using a glucose load containing the equivalent of 75 g anhydrous glucose dissolved in water. |
| OR |
| Hemoglobin A1C ≥6.5% (48 mmol/mol). The test should be performed in a laboratory using a method that is NGSP certified and standardized to the DCCT assay. |
| OR |
| In a patient with classic symptoms of hyperglycemia or hyperglycemic crisis, a random plasma glucose ≥200 mg/dL (11.1 mmol/L). |
Can Diabetes Cause High Blood Pressure?
High blood pressure, also called hypertension, is blood pressure that is higher than normal. Your blood pressure changes throughout the day based on your activities. Having blood pressure measures consistently above normal may result in a diagnosis of high blood pressure (or hypertension).
Diabetes and high blood pressure (hypertension) often occur together. When a person has more than one health condition at the same time, doctors refer to it as comorbidity. Conditions that are comorbid can influence each other.
Diabetes damages arteries and makes them targets for hardening, called atherosclerosis. That can cause high blood pressure, which if not treated, can lead to trouble including blood vessel damage, heart attack, and kidney failure.
A person with diabetes either does not have enough insulin to process glucose or their insulin does not work effectively. Insulin is the hormone that enables the body to process glucose from food and use it as energy.
As a result of insulin problems, glucose cannot enter the cells to provide energy, and it accumulates in the bloodstream instead.
As blood with high glucose levels travels through the body, it can cause widespread damage, including to the blood vessels and kidneys. These organs play a key role in maintaining healthy blood pressure. If they experience damage, blood pressure can rise, increasing the risk of further harm and complications.
There are three ways in which high glucose levels in the blood can increase blood pressure:
- The blood vessels lose their ability to stretch.
- The fluid in the body increases, especially if diabetes is already affecting the kidneys.
- Insulin resistance may involve processes that increase the risk of hypertension.
Controlling blood sugar levels and blood pressure can help prevent complications.
Sometimes, one condition can make the other worse or make a person more likely to get the other condition if they do not already have it. On the other hand, the steps that a person takes to manage one condition may help them manage (or even prevent) the other.
According to the American Diabetes Association (ADA), diabetes and high blood pressure can be comorbid conditions.
ADA data shows that:
- Nearly one in three American adults has high blood pressure.
- Two out of every three people with diabetes have high blood pressure or take prescription medications to lower their blood pressure.
Diabetes and high blood pressure both increase a person’s risk of heart disease (cardiovascular disease) by damaging the blood vessels and making the heart work harder to pump blood through the body.
It is estimated that adults with diabetes are nearly twice as likely to die from heart disease or stroke as people who do not have diabetes.
Diabetes Contributes to Hypertension
When blood sugars are elevated, it stresses the blood vessels. Damage to the inner linings of the vessels causes them to narrow and begin to accumulate plaque.
The plaque buildup narrows the vessels even more and forces the heart to work harder to pump blood throughout the body.
When the heart has to work harder, the force at which the blood pumps through the body increases, which leads to high blood pressure.
Plaque formation and buildup increase the risk of atherosclerosis—a condition that can increase the risk of heart attack, stroke, and peripheral arterial disease.
Complications
Both diabetes and high blood pressure can be managed through lifestyle changes. For example, a person with these conditions may benefit from being mindful about their diet, starting an exercise routine, quitting smoking, and losing weight.
When untreated or uncontrolled, both conditions can have serious health consequences, including cardiovascular disease, heart attack, stroke, peripheral arterial disease, and kidney disease.
- Cardiovascular disease is a general term for all diseases of the cardiovascular system. Complications of diabetes and high blood pressure can cause atherosclerosis, heart attack, stroke, and heart failure.
- Peripheral artery disease (PAD) is the hardening of the arteries in the legs, arms, head, or abdomen. Decreased blood flow from the heart to other parts of the body can cause pain and neuropathy. It can also lead to an increased risk of infection because of slow wound healing, death of tissue, and gangrene. People with diabetes and PAD are at increased risk of serious infections.
- Kidney disease can occur when high blood sugar or blood pressure causes constriction and narrowing of the blood vessels in the kidneys, which makes them weaker. The blood vessel constriction also reduces blood flow to the kidneys and causes damage. When damaged blood vessels are unable to do their job, they cannot filter and remove fluid and wastes. An excess buildup of fluid can cause blood pressure to get worse, which in turn causes more damage to the kidneys.
People with diabetes and/or hypertension sometimes need to take medication to help control the conditions and avoid complications.
ERECTILE DYSFUNCTION AND DIABETES
Erectile Dysfunction (impotence) — the inability to get or maintain an erection firm enough for sex is common in men who have diabetes, especially those with type 2 diabetes. It can stem from damage to nerves and blood vessels caused by poor long-term blood sugar control.
Erectile dysfunction (impotence) can also be linked to other conditions common in men with diabetes, such as high blood pressure and heart disease. Erectile dysfunction (impotence) might occur earlier in men with diabetes than in men without the disease. Difficulty maintaining an erection might even precede the diabetes diagnosis.
Having erectile dysfunction (impotence) can be a real challenge. It can leave you and your partner feeling frustrated and discouraged. Take steps to cope with erectile dysfunction — and get your sex life back on track.
Diabetes mellitus is one of the predominant risk factors of erectile dysfunction (impotence) and also one of the most difficult to treat. Approximately 50% of diabetic men will suffer from erectile dysfunction (impotence) within 10 years of the diagnosis. Erectile dysfunction (impotence) presenting in these men is widely regarded as a manifestation of more systemic vascular disease and is likely to precede a coronary event by 5 years. Combined with the prevalence of obesity and metabolic syndrome in these men, it is apparent that disease progression is likely to reduce the efficacy of conventional pharmacotherapeutic options for the treatment of Erectile dysfunction (impotence) in diabetic men. This has meant that diabetic men form a large group of patients undergoing end-stage treatment in the form of penile prosthesis surgery.
Our knowledge regarding the pathophysiology of Erectile dysfunction (impotence) in diabetes has gradually increased since the 1990s. As nitric oxide is the main erectile mediator, the field has focused on how diabetes alters the nitrergic and endothelial nitric oxide function.
MANAGEMENT AND PREVENTION OF DIABETES
Treatment options for elevated blood sugar and elevated blood pressure include a range of lifestyle changes and, in some cases, medication. The International Diabetes Federation (IDF) also suggests some organic products that can help people with this chronic condition:
Treating Type 2 Diabetes
Type 2 diabetes can sometimes be managed with lifestyle changes, including eating a healthy diet, getting more exercise, losing excess weight, and quitting smoking. You may also need to take insulin, as well as medications to manage related conditions like high blood pressure.
MANAGEMENT OF TYPE 2 DIABETES WITH LONGRICH PRODUCTS IN CAMEROON:
- Longrich NutriVrich Nutritious Drink in Cameroon
- longrich-cordyceps-militaris-in-cameroon
- Longrich Sea Buckthorn Berry Oil Softgels in Cameroon
- Longrich Classy Style Alkaline Cup in Cameroon
- longrich brown tea
- Longrich Vintage Liqour in Cameroon
- Longrich Cordyceps Militaris & Black Ginger Tablets in Cameroon
Longrich NutriVRich brown tea is hawthorn based, with aloe vera gel, supplemented by green tea, preventing pathogenic fire in addition to drying, protecting the liver and improving eyesight, promoting diuresis.
Both act as a fire-dispelling laxative, but also reduce liver fire, while promoting fat digestion.
Lipid-lowering, anti-atherosclerotic, anti-platelet aggregation effect, besides, it reduces body fat secondary absorption, effectively prevents excess heat.
The side compatibility scientific and rational, comprehensive regulation of human lipid metabolism physiology which, which plays lower cholesterol, triglycerides and other comprehensive lipid-lowering effect.
Suggested Use: Take 2 bags per day. Brew with boiled water and it can be re-infused for several times.
Storage: Seal and store in a cool dry place.
Ingredients: Green Tea, Semen, Cassiae, Polyghace Seche.
Treating Type 1 Diabetes
People with type 1 diabetes need to carefully monitor their glucose levels and take insulin to control their blood sugar. It’s also important to count carbohydrates, eat a balanced diet, and get regular exercise.
MANAGEMENT OF DIABETES WITH LONGRICH PRODUCTS IN CAMEROON:
TREATMENT & DOSAGE
- Nutri V Pink (1 per day)
- Cordyceps (1-2 per day)
- Berry Oil (2-3 per day)
Treating Prediabetes
Prediabetes can be slowed down or even reversed with lifestyle changes, including losing excess weight, eating a healthy diet, getting more exercise, and quitting smoking.
Treating Gestational Diabetes
Depending on what is causing gestational diabetes, you may be able to keep your blood sugar levels under control with diet and exercise, or you may need to take insulin.
Dietary Management
Eating to manage diabetes is not one-size-fits-all, but meal plans that focus on the quality and quantity of carbohydrates—as well as take into consideration a person’s lifestyle, culture, and food preferences—can help people with diabetes manage their blood sugar levels.
Eating for Diabetes
Carbohydrates are the macronutrient that affects a person’s blood sugar levels the most. When carbohydrates are metabolized, they turn into glucose.
Choosing fiber-rich carbohydrates—such as whole grains, non-starchy and starchy vegetables, and legumes—can help reduce blood glucose excursions, while also increasing feelings of fullness and optimizing vitamin, mineral, and antioxidant intake.
Studies have shown that following a plant-based diet, Mediterranean style of eating, or modified carbohydrate diet can help people manage diabetes and reduce their blood sugar.
A good rule is to aim to eat two to three cups of non-starchy vegetables daily or to make half of your plate non-starchy vegetables at each meal.
COMPLICATIONS OF DIABETES:
If it is not controlled, diabetes can cause a host of complications that can affect nearly every organ in the body. Diabetes complications include:
- Heart disease
- Stroke
- Kidney disease
- Nerve damage
- Eye damage
- Digestion problems
- Erectile dysfunction
- Skin problems
- Infection
- Dental problems.